Nerve Blocks for Management of Pain Following Hip Fracture
November 2019
Click here to watch this entire event from this month’s Journal Club
Vignette
You’re moonlighting in an austere emergency department, and the night has
been relatively benign except for your poor 79-year-old severely demented
patient who suffered an isolated mid-shaft femur fracture from a mechanical fall
earlier today. Unfortunately, the patient is also morbidly obese and has OSA
requiring CPAP at night when sleeping. The patient is miserable and is now
making your staff miserable, howling out in pain with every breath. Opioids aren’t
touching the searing pain, and now you’re worried about potential respiratory
complications from too much of a good thing. Your off-going partner in crime
mentions doing a “nerve block” and everyone lets out a sign of relief. But what
nerve block? And will it work? You nod smartly in agreement and excuse yourself
to the bathroom to check out some online resources…
PICO Question
Population: Elderly patients with acute hip fracture in the emergency department
Intervention: Regional nerve block with any local anesthetic for analgesia
(femoral nerve block, 3-in-1 nerve block, or fascia iliaca block)
Comparison: Standard pain management strategy without regional nerve block
Outcome: Pain scores during ED length of stay, time to effective analgesia,
incident delirium, opioid side effects (hypotension, vomiting, delirium), anesthetic
toxicity (dysrhythmia, confusion, hypotension), regional nerve block adverse
consequences (delayed rehabilitation)
Articles
Article 1: Riddell M, Ospine M, Holroyd-Leduc JM. Use of Femoral Nerve Blocks to Manage Hip Fracture Pain among Older Adults in the Emergency Department: A Systematic Review. CJEM. 2016 Jul;18(4):245-52
ANSWER KEY
Article 2: Fletcer AK, Rigby AS, Heyes FL. Three-in-one femoral nerve block as analgesia for fractured neck of femur in the emergency department: a randomized, controlled trial. Ann Emerg Med. 2003 Feb;41(2):227-33
ANSWER KEY
Article 3: Morrison RS, Dickman E, Hwang U, et al. Regional Nerve Blocks Improve Pain and Functional Outcomes in Hip Fracture: A Randomized Controlled Trial. J Am Geriatr Soc. 2016 Dec;64(12):2433-2439
ANSWER KEY
Article 4: Sharma S, lorio R, Specht LM, Davies-Lepie S, Healy WL. Complications of femoral nerve block for total knee arthroplasty. Clin Orthop Relat Res. 2010 Jan;468(1): 135-40
ANSWER KEY
Bottom Line
Epidemiology of Hip Fractures
Aging populations worldwide mean that adult emergency departments care for
increasing proportions of older trauma patients each year. Currently, adults over
age 65 represent 23% of trauma admissions and traumatic injury is the 5th
leading cause of geriatric mortality. Older adult trauma costs $34 billion in direct
medical costs annually with 75% of those expenses related to traumatic brain
injury and lower extremity injuries. Standing level falls are the most common
injury mechanism with almost 30,000 fall-deaths in 2016 alone. While fall
prevention is an emergency medicine resident core competency and an essential
component of the ACEP/SAEM/AGS/ENA Geriatric Emergency Department
Guidelines, high-quality reviews on this topic already exist and the Wash U EM
Journal Club has critically appraised this literature in 2014.
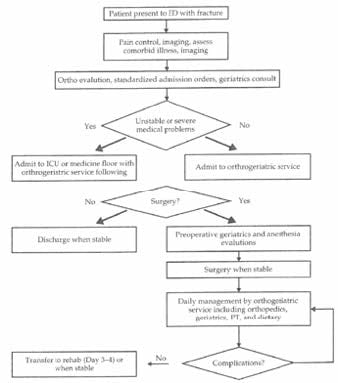
More than 250,000 adults over age 65 are hospitalized annual in the United States due to a hip fracture – a number projected to increase to 289,000 by 2030. Operative delays increase mortality, but assessing concurrent injuries and medical stability for surgery requires time and expertise. Increasingly Orthogeriatric co-management care models are being used as illustrated in this figure (from De Jonge 2001 and page 296 of Geriatric Emergencies – A Discussion Based Review). Acute co-management models of hip fracture patients typically includes emergency medicine, trauma, internal medicine, geriatrics, anesthesia, and orthopedic surgery. These co-management models significantly reduce hospital length of stay, surgical delays, complication rates, and mortality (Friedman 2008, Biber 2013, Grigoryan 2014). Two of the complications reduced by this model are oligoanalgesia and delirium.
Older Adult Oligoanalgesia – A Risk for Delirium Approximately 10% of patients over age 65 experience delirium during an episode of emergency department care. Pre-operative cognitive impairment and inadequate analgesia are both associated with incident delirium following hip fracture, partially because assessing pain is challenging in patients with severe dementia. Unfortunately, despite the availability of feasible and valid instruments dementia is rarely recognized in ED settings (Carpenter 2011, Carpenter 2019) and transdisciplinary consensus about how to identify or intervene upon occult cognitive impairment is lacking. Pre-operative delirium also increases the risk of post-operative delirium (Agrawal 2020) and related complications including mortality (Hamilton 2017). Reducing hip fracture-associated delirium in the emergency department requires a multi-component intervention and regional
nerve blocks are one of those components.
Regional Nerve Blocks Nerve blocks for femoral neck (hip) fractures have been described for decades (Finlayson 1988, Haddad 1995, Cochrane Review 2002). Similar to airway management, initially regional nerve blocks were the domain of anesthesiology alone. However, geriatric emergency medicine advocates highlighted the value of regional nerve blocks over a decade ago (Carpenter 2013). Three types of hip fracture nerve blocks have been described: femoral, 3-in-1, and fascia iliaca. None of these techniques is clearly superior to another. Historically, landmarkbased approaches were used, but point-of-care ultrasound (POCUS) is now the standard and requires pre-procedure training. Even with POCUS errors can occur as recently illustrated in ACEP Now by placing the probe too distal in the thigh (Figure 4) or not perpendicular to the femoral artery (Figure 5). Another essential component of ED regional nerve blocks that was not discussed at Journal Club is the necessity to document a thorough motor-sensory neurological exam prior to the nerve block because neurological findings will be obscured after the regional block. The timing of this distal motor-sensory exam should be agreed upon with surgical consultants prior to launching a regional nerve block protocol. One approach to standardize documentation would be to insert
mandatory motor-sensory exam findings into the regional nerve block procedure
note.
Bupivacaine Precautions
Bupivacaine is described in most regional nerve block studies. The July 2019
issue of EM:RAP reviewed concerns about bupivacaine toxicity with the following recommendations. 1) Withdraw to ensure not in vascular structure before injecting and repeat withdraw after every 5-10 mL to ensure you haven’t drifted into a vessel; 2) hydrolocate with POCUS before you inject; 3) be aware that the 20-30 mL of 0.25% to 0.5% bupivacaine required for hip fracture nerve blocks can induce cardiotoxicity including hypotension and seizures – since lidocaine does not have this cardiotoxicity or neurotoxicity consider using lidocaine rather than bupivacaine; and 4) don’t use bupivacaine without intralipid nearby (in the ED).
Journal Club Discussion Between Geriatric Trauma & Emergency Medicine
Here is the synopsis of the Journal Club discussion between Geriatric Trauma and Emergency Medicine, including Dr. Jason Snyder from Trauma Surgery.
PGY-I
This was the only systematic review evaluated. Meta-analysis was not performed due to differences in regional nerve block methods used and pain assessment techniques. Seven ED-based RCT’s of overall low quality demonstrate immediate and sustained pain relief with either single femoral nerve block or continuous catheter infused femoral nerve block. In addition, less rescue opioid analgesia is required. For now, the benefits appear to outweigh the risks so femoral nerve blocks merit consideration in the setting of older adult hip fractures.
PGY-II
This was a UK-based randomized controlled trial. Landmark-based 3-in-1 nerve blocks by trained ED physicians effectively alleviates hip fracture pain in non-cognitively impaired older adults. These results cannot be extrapolated to patients with dementia or delirium, which is unfortunate since cognitively frail individuals are theoretically more likely to benefit from more efficient analgesia in terms of reduced incident delirium and the corresponding morbidity associated with delirium (increased ED length of stay, operative delay, increased hospital length of stay, higher healthcare costs). In addition, this study cannot address whether ED nerve blocks for hip fracture delay rehabilitation. Since this study was published, alternative nerve block approaches such as the fascia iliaca block have also proven effective and feasible so future research could compare the efficacy and physician-level acceptability of different nerve block techniques.
PGY-III
This was a randomized controlled trial from three New York city hospitals. In a largely Caucasian population, emergency medicine residents with structured point-of-care ultrasound training to administer femoral nerve block with bupivacaine followed by pre-operative Anesthesia continuous fascia iliaca block with ropivacaine, reduces pain immediately and in the first days of post-operative recovery at rest or with movement. In addition, functional recovery improves with less missed physical therapy time, lower morphine equivalentsrequired, and less opioid side effects.
PGY-IV
This study was included because of local Washington University surgical concerns about delayed post-operative rehabilitation following emergency department POCUS regional nerve blocks for hip fracture patients. Since none of the hip fracture regional nerve block studies reported the outcome of delayed rehabilitation (the PGY-III manuscript reported an improvement in rehabilitation completion rates), this retrospective review of knee arthroplasty cases was discussed. The cohort was not randomized but was analyzed as a subset receiving pre-operative femoral nerve block compared with a subset who did not.
Although this study indicates a concerning trend towards increased falls following femoral nerve block for knee arthroplasty patients, extrapolating these concerns to hip fracture patients in the ED is problematic. First, hip fracture patients are generally older with present with the possibility of multiple trauma and are often cognitively frail at risk of pain-induced delirium related to oligoanalgesia. On the other hand, knee arthroscopy arthroplasty patients are generally more medically stable with less co-morbidities and with more time to titrate analgesia. In other words, most arthroplasty patients are not frail. If a femoral nerve block
contributes to falls or imbalance in someone who has been indicated for elective surgery, clinicians should be concerned that more frail urgent surgical patients are less able to overcome subtle quadriceps weakness. Additional considerations in weighing the potential risks/benefits of regional anesthesia include the time course of the local anesthetic and technique performed. If the effect is gone by 24 hours, any real clinically significant delay in rehab is unlikely (and ER -> OR -> recovery -> first PT session would RARELY occur in less than
24 hours). The follow up question is whether the fascia iliaca block works as well in pain control with less quad weakness, which takes better research to compare the two in this population. Second, contemporary ED practice is POCUS femoral nerve block rather than nerve stimulator. Despite these limitations, the results do not highlight sufficient risk to merit avoiding femoral nerve blocks. The concerning preponderance of falls amongst femoral nerve block patients highlights the need for a post-operative fall prevention protocol including
monitoring for delirium. In pre-op ED settings, there is rational to support nerve blocks as a method to reduce pain-related delirium, but this is still being evaluated in ED studies.
Future Research Priorities
Research is still needed! Fortunately, Jacques Lee from the Schwartz-Reisman Institute is completing a multi-institutional cluster randomized controlled trial in early 2020. Future emergency medicine femoral nerve block investigators should
- Identify patients most likely to benefit from regional nerve blocks since ultrasound experts like Chandra Aubin opined that these blocks should not be used on every hip fracture patient due to potential adverse effects and continuous operational time constraints;
- Include patients with prevalent delirium and identified dementia using ethical approaches to obtain consent;
- Standardize pain assessment measures and intervals;
- More holistically using emergency medicine validated instruments report patient characteristics, including: dementia, frailty, co-morbid illness burden, injury severity, and incident delirium;
- Explicitly characterize femral nerve block operator’s use of POCUS and level of expertise/training with femoral nerve blocks and;
- Contemplate additional potential patient-centric (beneficial and adverse) outcomes in conjuction with Geriatric Trauma, Ortho-Trauma, Anesthesiology, and Rehabilitation researches and clinicians. For example, some surgeons believe that ED regional nerve blocks delay initiation of post-operative rehabilitation. Future investigators will need to evaluate whether post-operative rehabilitation is delayed by ED POCUS regional nerve blocks for hip fracture because existing studies have not evaluated that outcome.
- Explore cost-effectiveness of regional nerve blocks for hip fracture using various models, including mobile POCUS team, nurse-led service, general EM physicians and physician extenders, or anesthesiology;
- Describe implementation science approaches to identify and overcome common barriers to widespread adoption of regional nerve blocks
Bottom Line: The benefits of regional nerve blocks (mostly femoral nerve blocks) outweigh the risks in emergency department settings. Benefits include immediate and sustained pain relief in addition to lower rates of missed physical therapy and less opioid-related side effects. Appropriate patients in whom to consider regional nerve blocks include those at increased risk of delirium (frail, cognitively impaired), borderline low blood pressures, and inadequate analgesia after reasonable opioid dosing.